Toxic Drugs Are Circulating
In 2016, the Province of British Columbia declared a public health emergency in response to a significant increase in drug-related overdoses and deaths. This toxic drug crisis, primarily driven by a highly potent and unregulated supply of illicit drugs, remains a complex and evolving issue.
Over the past eight years, more than 15,000 lives have been lost in B.C. due to toxic drugs. BC Coroners Service data indicates that First Nations people died of drug poisonings at 6.1 times the rate of other B.C. residents in 2023.
Substances, or drugs, can be defined as something that alters your mental, emotional or physical state. Legal substances, such as alcohol, cannabis, caffeine, prescriptions & nicotine are commonly used. Illegal substances are not regulated and carry higher risks as you may not know the exact contents.
It is important to think about the impacts that substance use can have on your health and wellbeing. There are increased risks associated with using substances. Please consider ways to stay safer if you or someone you know uses drugs or is considering trying drugs for the first time.

Alcohol
What is alcohol?
Alcohol is a depressive substance that can alter your mental, physical and emotional health. Alcohol is a legal substance in Canada and can be purchased in British Columbia by an adult over the age of 19.
Canada's Guidance on Alcohol and Health, defines a standard drink as:
- 1 beer, cooler, cider or premixed cocktail (341mL or 12oz, 5% alcohol); or
- 1 glass of wine (142ml or 5oz, 12% alcohol); or
- 1 drink of distilled alcohol (43ml or 1.5oz, 40% alcohol)

Learn More
How alcohol can impact you
All alcohol has the same effect on the body, and no amount of alcohol is good for your health. The more you drink, the more consequences you could face.
Consuming four or more standard drinks in one setting as a woman, or five or more standard drinks as a man, is considered binge drinking. A high proportion of alcohol consumed by university students is binge drinking, often while celebrating or socializing with friends.
There are significant risks associated with long-term, excessive binge drinking, including developing different types of cancer and an increased risk of heart disease and stroke.
Short-term alcohol use can:
- Impact your judgement, reflexes, and behaviour
- Increase your risk of anxiety, depression, suicide, and other mental health concerns
- Decrease your academic performance
- Increase your risk of injury from violence, accidents, or risky behaviours
- Increase your risk of developing health issues such as cancer and heart disease
Visit the Canadian Centre for Addiction & Mental Health for more information about alcohol’s effects.
Signs of alcohol intoxication and poisoning
If someone consumes an excessive amount of alcohol, they can experience alcohol poisoning. This can lead to irreversible brain damage or death if not treated immediately.
Alcohol Intoxication
- Flushed skin
- Slurred speech
- Staggering gait
- Impaired judgment
- Inability to focus or pay attention
- Reduced inhibition and muscle control
Alcohol Poisoning
- Inability to stand
- Vomiting
- Incontinence
- Clammy skin
- Low body temperature
- Slow or labored breathing
- Passing out or inability to wake
- Seizures
Ways to stay safe and reduce harms while drinking
If you choose to drink alcohol, here are some ways to stay safe:
- Eat food and drink water before and while consuming alcohol
- Choose beverages with lower alcohol content and alternate drinks with water or soda
- Stop drinking before you feel intoxicated
- Drink slowly and avoid drinking games
- Do not mix alcohol with other substances
- Arrange safe transportation home or a safe place to stay overnight
- Do not drink and drive
Additional resources and supports
- Alcohol and Drug Information & Referral Service — 1-800-663-1441
- Government of BC – Help Starts Here
- BC Mental Health & Substance Use Services
- Canada’s Guidance on Alcohol and Health
- Saying When App
Support groups
Vaping and E-cigarettes
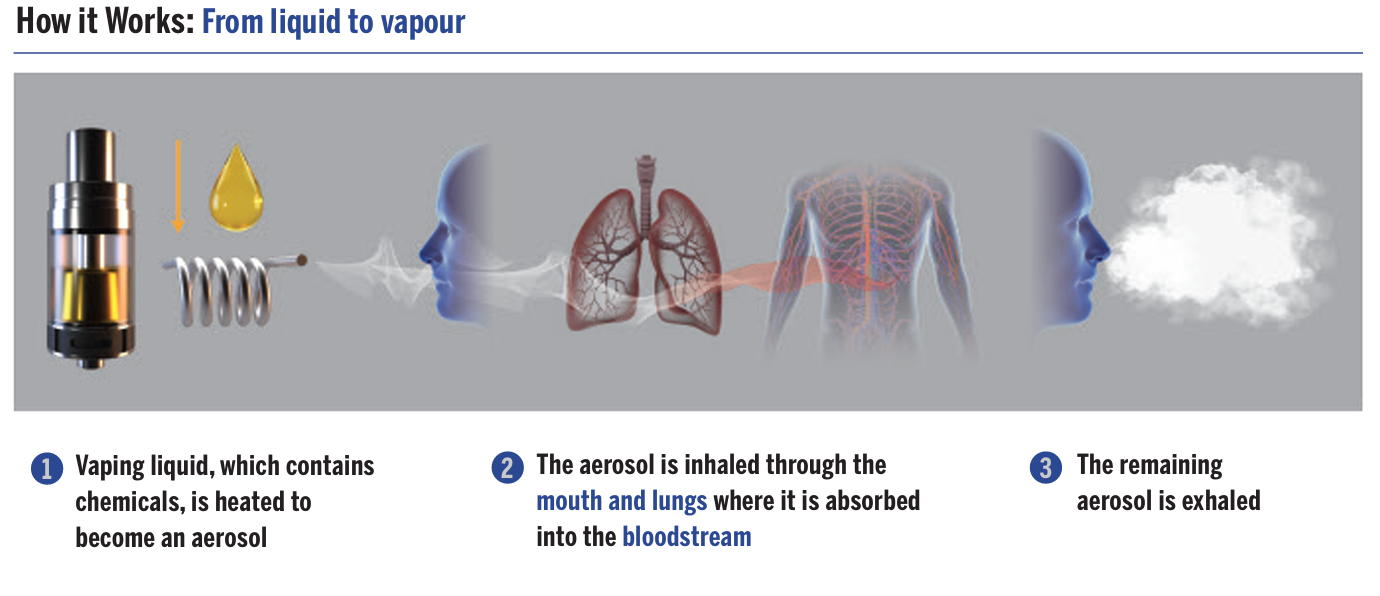
Electronic cigarettes, or vapes, are small, handheld battery-powered devices used to inhale an aerosol. It’s similar to smoking a cigarette, but vaping heats liquid rather than burning tobacco. The term “vaping” can also refer to the inhalation of cannabis. For more information on cannabis, visit Cannabis on Campus.
Vaping devices come in all shapes and sizes.
Types of vaping devices
- Open systems: The vape is filled manually by adding vaping liquid into a tank or pod.
- Closed systems: The device holds a disposable cartridge or pod that is pre-filled with vaping liquid.
Visit Health Canada to learn more about the mechanics of vaping.
Most vaping liquids sold are flavoured and contain nicotine, along with a variety of other chemicals depending on the product. Visit Health Canada for more information about vaping.

Learn More
Nicotine
Nicotine is a highly addictive substance found in tobacco leaves. It releases natural chemicals in your brain that can make you feel more alert, energized or calm. With prolonged use, your body builds a tolerance to some of these effects which can lead to increased use and dependence. Many individuals experience withdrawal symptoms if they go without nicotine for too long. These symptoms go away only after consuming more nicotine or permanently quitting.
Withdrawal symptoms may include:
- Dizziness and shakiness
- Headaches
- Anxiety and irritability
- Nervousness and restlessness
- Difficulty concentrating and sleeping
- Increased appetite
- Slight depression or feeling down
- Cravings for more nicotine
According to Health Canada, most withdrawal symptoms occur during the first week and are usually gone within two to four weeks.
Other health risks
Currently, there is not enough data to know the long-term effects of vaping. However, short term effects include wheezing, shortness of breath and chest pain. Vaping irritates the lungs and airways and can be especially harmful to individuals with underlining health conditions such as asthma. Vaping can also harm the heart by impacting arteries and blood vessels, increase heart rate and blood pressure. Lastly, vaping liquid contains chemicals that are toxic and cancer-causing.
Guidelines and harm reduction
Should you choose to continue vaping despite the risks, these e-cigarette guidelines and recommendations can help you to reduce the risks:
- Do not use unlabelled or old products
- Use your vape device on low heat to reduce inhaling more harmful chemicals
- Be aware of how much nicotine you are consuming to prevent nicotine sickness
- Be careful how you store your vaping device and liquids to prevent nicotine poisoning
- Avoid or limit long term use of vapes
- Maintain your vaping device (clean the vaping tank, change the vape coil regularly, etc.)
- Avoid modifying or reusing disposable vapes
- Store your vape battery carefully to prevent fires or explosions
Smoking cessation
In British Columbia, residents are eligible for a 12-week supply of nicotine replacement therapy (nicotine patches, gum, lozenges) or prescription medication. Nicotine replacement therapy is available at most pharmacies without a prescription. For all prescription medications, please talk to your doctor.
Resources to help you quit smoking or vaping
- HealthLink BC: Quit Smoking
- QuitNow Helpline – a free service with coaches to help you quit and stay smoke-free
- BC Smoking Cessation Program - This program covers the costs of prescription and non-prescription smoking cessation aids for BC residents
- There are two Fraser Health Authority clinics and one Vancouver Coastal Health clinic that provides smoking cessation services to residents in their regions
There are two Fraser Health Authority clinics and one Vancouver Coastal Health clinic that provide smoking cessation services to residents in their regions.
Cannabis
Cannabis, also known as weed, pot, or marijuana, is a plant containing hundreds of chemical substances that affect the brain and body, including THC and CBD. THC is a psychoactive substance found in cannabis. It is responsible for the “high” and intoxicating effects you feel after using cannabis. CBD is another common substance found in cannabis, but it is not psychoactive. CBD is being researched for its possible therapeutic properties. Cannabis can come in many forms, including dried flower/leaves, hash oils, extracts (shatter), edibles, and topical creams. Cannabis products can be smoked, vaped, consumed or applied topically.
- Even though recreational cannabis is legal in Canada, it is illegal to transport cannabis across the Canadian border. You could be charged with a criminal offense. You can also be denied entry and/or banned from entering your destination country if you admit to previously using recreational cannabis while in Canada. It is your responsibility to inform yourself about the laws of the country you are travelling to.
- If you are a temporary resident of Canada (i.e.: international student, exchange student, or visiting student) and have been convicted of a cannabis-related offense, you could be considered inadmissible to Canada. This could also result in deportation from Canada. You could also face prosecution in your home country. For more information about this, please visit: Government of Canada - New Impaired Driving and Cannabis Related Penalties could affect immigration status
To explore more information about Cannabis in British Columbia, please visit: cannabis.gov.bc.ca

Legalization in Canada
On October 17th 2018, the recreational use of cannabis became legal in Canada. In 2019, federal cannabis regulations allow the production and sale of edible cannabis products, cannabis extracts and cannabis topicals.
On KPU Campuses
In accordance with KPU’s Smoke Free Campuses and Properties Policy (SR3), smoking and vaping is prohibited on all KPU campuses and properties, including inside private vehicles. This now includes recreational cannabis.
In accordance with KPU’s SR1 Policy, “Students under the influence of alcohol or non-medical drugs must be refused entry to instructional settings if their condition can constitute a hazard to themselves or others”. KPU students are expected to treat recreational cannabis and cannabis products similar to alcohol and other drugs and not come to campus while impaired.
BC Laws

You must be 19 or older to buy, use or grow recreational cannabis.

Recreational cannabis and cannabis products can only be legally purchased at government-run stores, licensed private retailers, or on the online BC store.

Adults can possess 30 grams of dried cannabis, or its equivalent, in public.

Many public spaces in BC do not permit smoking and vaping cannabis, such as parks, bus stops and public buildings.
Opioids
Opioids are a type of psychoactive substance with depressive (or downer) effects. Opioids may be prescribed or used illegally to reduce pain and manage opioid dependence, and can make people feel sleepy, euphoric, or relaxed. They also slow down body systems like breathing and impact the body's ability to maintain normal function. Some examples of opioids include: codeine, hydromorphone, fentanyl, heroin, morphine, methadone, oxycodone, and percocet.
Since opioids produce "euphoria" like effects, they have the potential for higher-risk use, such as:
- taking an illegally obtained or produced opioid, like heroin or fentanyl
- using an opioid medicine improperly (taking more than prescribed or at the wrong time)
- using an opioid medicine that wasn't prescribed to you
An opioid drug poisoning occurs when you take too much of an opioid and a toxic amount attach to receptors in the central nervous system. When you take more than your body can handle, breathing slows and this can lead to unconsciousness and even death. If you are struggling with opioid use, help is available.
If you are looking for treatment for substance use
- If you are looking for treatment for substance use, contact the Opioid Treatment Access Line at 1-833-804-8111. They are open daily, 9 AM to 4 PM, with the last intake at 3:30 PM and voicemail available after hours.
- It is important for you to consider ways to stay safer if you—or someone you know—uses drugs or is considering trying drugs for the first time. No unregulated drug is safe. Prescription medications should also be treated with caution. Visit Help Starts Here for support with reducing or stopping substance use.

Naloxone Kits and Harm Reduction
- If you use or intend to use unregulated drugs, go slowly, pace yourself, and use around other people.
- Sign up for Toxic Drug Alerts in your region by texting the word JOIN to 253787.
- Download the Lifeguard Connect App (Apple App Store or Google Play Store). This app connects you with emergency responders if you or someone you know becomes unresponsive.
- Carry naloxone and sign-up for a free Naloxone training session.
- Consider having your drugs checked. You can get your drugs tested at supervised consumption sites or overdose prevention sites for free. Visit drugcheckingbc.ca to find access to drug testing and testing strips.
Where you can find Naloxone on campus:
Naloxone is available at all KPU locations in the event of an emergency:
- KPU Surrey – Maple building & Cedar building
- KPU Langley – East building & West building
- KPU Richmond – First floor Main Building
- KPU Tech – Main Building
- KPU Civic – Level 7 & Level 8
Always call 9-1-1 first in the event of an emergency. Naloxone should be given to an unresponsive person showing signs or symptoms of an overdose. For more information about naloxone, visit KPU First Aid. There are also Emergency Call Buttons across KPU campuses that serve as direct service lines to Security and First Aid.
*NEW: Naloxone Pilot Program at the KPU Surrey Library
In response to the province's toxic drug crisis, the B.C. Ministry of Health has provided KPU with naloxone kits for public distribution. This pilot program will run until the end of the 2026 calendar year!
The naloxone distribution desk will be located at the KPU Surrey Library, first floor of the Arbutus building, near the Information Desk. Library staff and KPU security will be monitoring and restocking the supply.
The naloxone kits are intended to be taken by members of the KPU community for use off-campus in case an overdose is encountered. To learn how to administer naloxone, explore the workshops and resources section of this webpage!

Frequently Asked Questions
What is the Naloxone Pilot Program?
The Naloxone Pilot Program is a $50-million response from the B.C. Ministry of Health to the province’s toxic drug crisis. KPU has been provided with naloxone kits for public distribution. The pilot program will run until the end of the 2026 calendar year
Where is the Naloxone Pilot Program located at KPU?
The naloxone distribution location will be at the KPU Surrey Library, first floor of the Arbutus building near the Information Desk.

What should I do if I see an overdose on campus?
In the event of a suspected overdose or other medical emergency on campus Call 911 immediately, then contact First Aid or KPU Security. Acting quickly can save a life.
Who is responsible for overseeing the Naloxone Pilot Program?
Library staff and KPU Security will be monitoring and restocking the naloxone distribution location.
Has there been a history of harmful drug use at KPU?
No. KPU has not had any history of harmful drug use on campus by KPU students or employees. The kits are indented to be taken by members of the KPU community for use off-campus, in case an overdose is encountered.
Are there any safety concerns resulting from the program?
No. The naloxone distribution site is in a highly visible location in the Surrey Library and will be monitored. KPU security will be on hand to respond appropriately should an incident take place.
How does Naloxone work?
You can find details here: Training, Naloxone, Narcan, overdose, drug poisoning | Toward the Heart
Where can I learn more about naloxone and B.C.’s toxic drug crisis?
You can find more information on KPU’s Substance Use - Harm & Overdose Prevention webpage, or on the BC Centre for Disease Control’s harm reduction services site Toward The Heart
Responding to an accidental opioid poisoning
If you think someone is experiencing an accidental opioid poisoning, call 9-1-1 right away. Stay with that individual until first responders or KPU first aid and security arrive.
Potential signs of an opioid poisoning
- Not moving and can’t be woken up
- Slow breathing or not breathing at all
- Choking, gurgling sounds or even snoring
- Blue lips and nails
- Cold or clammy skin
- Tiny pupils
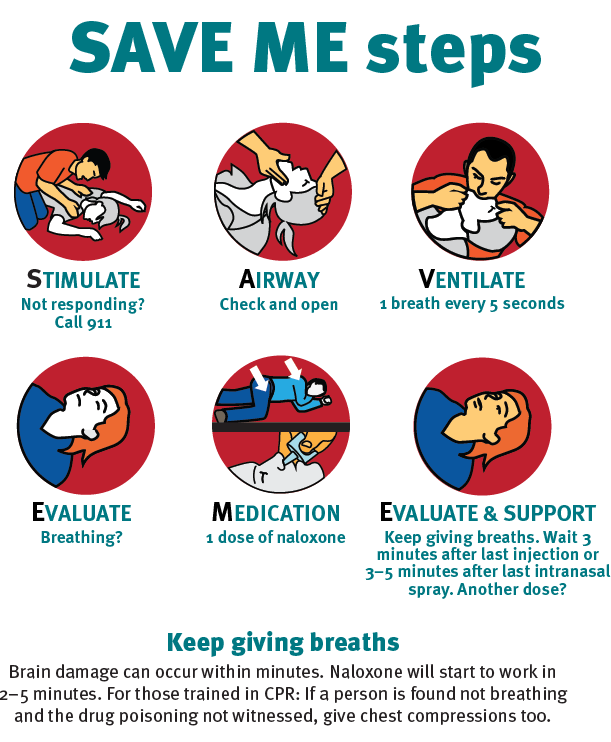
Use the SAVE ME steps to provide aid while you are waiting for help to arrive:
- Stimulate: Not Responding? Call 9-1-1.
- Airway: Check and open.
- Ventilate: One breath every five seconds.
- Evaluate: Breathing?
- Medication: One dose of naloxone.
- Evaluate and support: Keep giving breaths. Wait three minutes after the last injection or three to five minutes after the last intranasal spray. Another dose?
Brain damage can occur within minutes. Naloxone will start to work in two to five minutes. For those train in CPR: if a person is found not breathing and the drug poisoning not witnessed, give chest compressions too.
If you do not know how to administer naloxone or do not have access to it, continue giving breaths until help arrives.
Resources and Workshops
- In an emergency, CALL 9-1-1. KPU also has Emergency Call Buttons that are a direct link to Security and First Aid across campus.
- Opioid Treatment Access Line: 1-833-804-8111
- BC Alcohol & Drug Information and Referral Service: 1-800-663-1441
- Suicide Crisis Helpline or call 9-8-8
- Toward the Heart (information about opioids, naloxone and harm reduction)
- Free Naloxone Training
- Respond to Overdose (information on overdose prevention and response)
- Health Canada Substance Use Toolkit for Young Adults
- HealthLinkBC or call 8-1-1
- Here2Talk (free mental health support for BC university students
- KUU-US Crisis Line Society or call 1-800-599-8717
- First Nations Health Authority (harm reduction resources)
- Crisis Centre of BC or call 310-6789 (mental health and crisis response)
- TELUS Student Support App (free mental health support for KPU students)
- Help Starts Here BC (BC health, mental health and wellness services)
- Foundry BC (health and wellness services for young people ages 12-24)
- Building Better Mental Health and Addiction Care (information and resources on mental health and addictions)

Decriminalization Has Ended in BC
The Government of British Columbia announced the end of the decriminalization pilot program on January 31, 2026. This means that as of February 1, 2026, possession of any amount of illicit substances in any place that does not have a specific exemption (like a supervised consumption site) will be illegal.
If you have any amount of illicit substances in your possession, they may be seized, and you may be arrested, charged and convicted.
Law enforcement official continue to have discretion to use non-criminalizing approaches to substance use when public safety is not impacted. This might include providing public health information, voluntary referrals, or other supportive approaches.
Learn More
Supervised consumption, overdose prevention, and drug checking services provide harm reduction supports such as witnessed consumption, drug poisoning response, and confirming the contents of substances. Policies supporting these services are separate from the decriminalization exemption. These services were in place before the decriminalization pilot and their legal status has not changed with the end of the exemption.
The Good Samaritan Drug Overdose Act is also separate from decriminalization. You will be protected from simple possession charges if you are getting help for an overdose.
For more information, visit www.towardtheheart.com


The Good Samaritan Act
Saving a life is the number one priority during an opioid poisoning.
The Good Samaritan law protects you from simple drug possession charges and violations of conditions related to parole, probation, conditional sentences or pre-trial release.
This law applies to the person who has overdosed, the person who seeks help and anyone at the scene when help arrives. Visit Health Canada for more information about the Good Samaritan Drug Overdose Act.









